
Stone Age:
Crude tools used to cut vessels & drain out blood
Middle Ages
Barber-surgeons performed bloodletting & leeching
Bleeding bowl: used to collect blood from patient
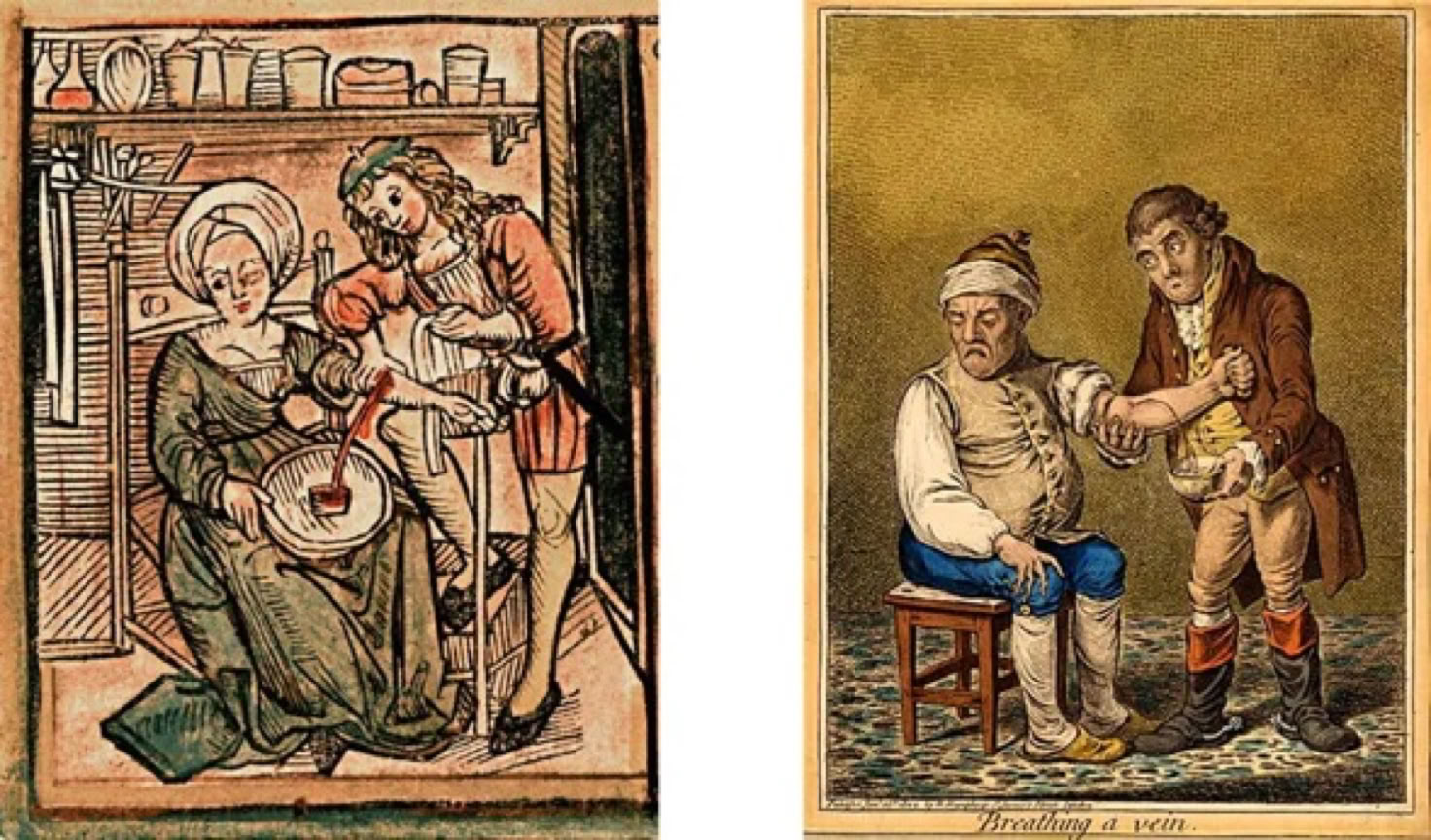

17th & 18th Centuries
Phlebotomy became a major therapy
Lancets & fleams were used to cut veins & arteries
Cupping & leeching were used
Single or double-edged blade

Multiple fleams attached & folded for ease of carrying, then the blades wiped clean with a rag
Art of Cupping
- Application of heated suction device, the cup
- Incision with a fleam (lancet)

Leeching
- Place drop of milk or blood on the patient's skin
- Introduce Hirudo medicinalis to the site that injects:
• Local vasodilator
• LocaI anesthetic
• Hirudin, an anticoagulant
• Present day
- Used in microsurgical replantation
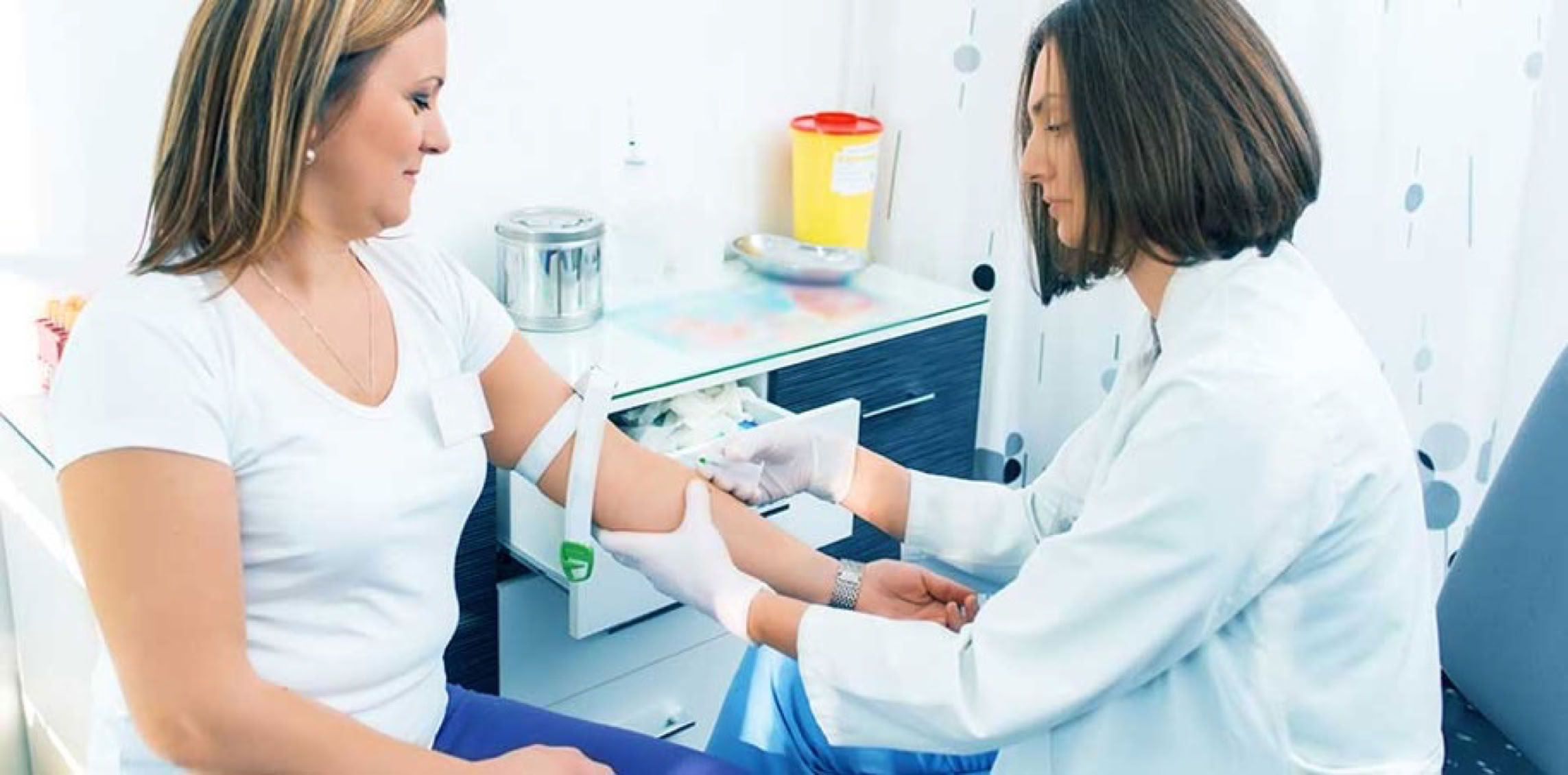
MODERN PHLEBOTOMY
Modern phlebotomy shares little more than a name with these ancient practices.
Today, phlebotomy is performed primarily for diagnosis and monitoring of a patient's disease condition, and it involves highly developed and rigorously tested procedures and equipment to ensure the safety and comfort of the patient and the integrity of the sample collected.
Goals and Methods of Phlebotomy Today
Remove blood for transfusions at a donor center
Remove blood for therapeutic purposes (polycythemia)
Obtain blood for diagnostic purposes & monitor treatment
Methods
Venipuncture: blood collection via a needle inserted in a vein
Capillary puncture: blood collection via skin puncture

Patient-Client Interaction
Customer Relations
- Phlebotomist may be the only contact the patient has with lab
- Patient may judge hospital based on encounter with phlebotomist

Goal: put patient at ease & establish positive relationship
Qualities of Professionalism
• Professional appearance
• Self-confidence
• Integrity
• Compassion
• Dependability
• Ethical behavior
Confidentiality
• Patient information must be kept private & confidential
• Ethical standards & laws enforce confidentiality
• Health Insurance Portability & Accountability Act (HIPAA)
• Disclosure of PHI requires written authorization

Communication Skills
Communication: The manor by which information is exchanged or transmitted
Verbal
- Active listening
- Nonverbal (body language)
Kinesics: study of nonverbal communication
Proxemics: use of space
• Appearance
• Touch
Elements of Effective Healthcare Communication
- Empathy
- Control
- Respect & confirmation
- Trust


Starts when you receive the order
Clinical Laboratory Improvements Amendments of 1988
-Federal regulations passed by Congress
-Establish quality standards standards that apply to all laboratories
It sets standards such as:
-Quality assurance
-Quality control
-Proficiency testing
-Personnel qualifications
Quality Phlebotomy consists of a set of Policies and Procedures designed to ensure the highest-quality patient care and consistent specimen analysis.
Patient preparation, specimen collection, and transporting procedures are critical areas for quality phlebotomy.
Quality Control ensures all equipment used is being monitored, such as regular inspection and calibration of equipment to ensure accurate tests results.
Quality Assurance means that all phlebotomists and personnel are following procedures and guidelines when performing techiques
*Remember: The Terms Quality Control and Quality Assurance are NOT interchangeable.
Phases of a blood draw
Three phases of phlebotomy:
1.Preanalytical
2.Analytical
3.Postanalytical
The Preanalytical phase:
Ends when the needle touches the skin

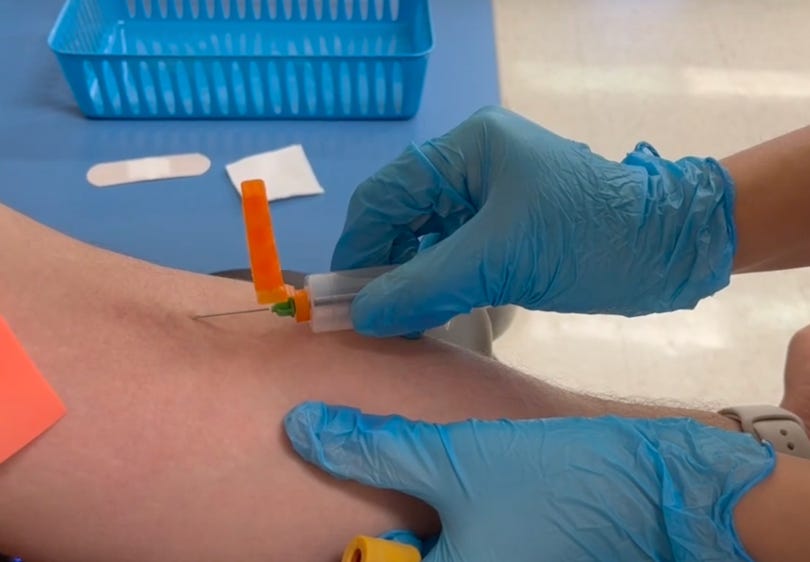
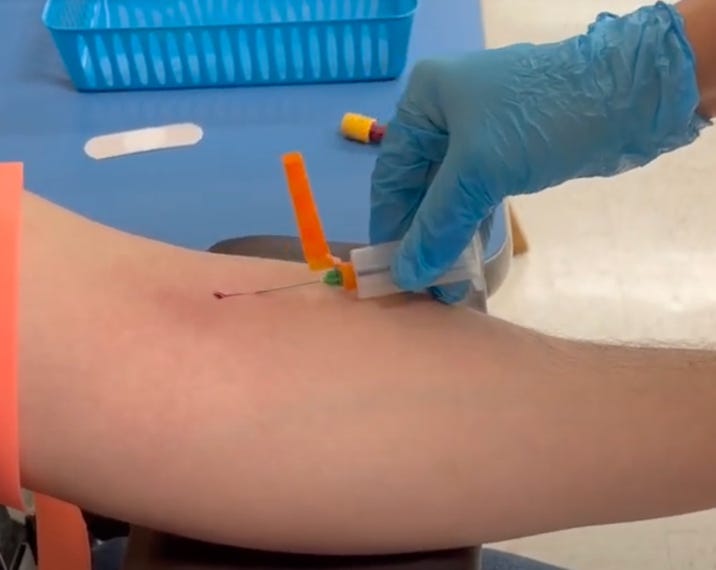
The Analytical phase:
Starts when the needle touches the skin
Ends when the needle leaves the skin
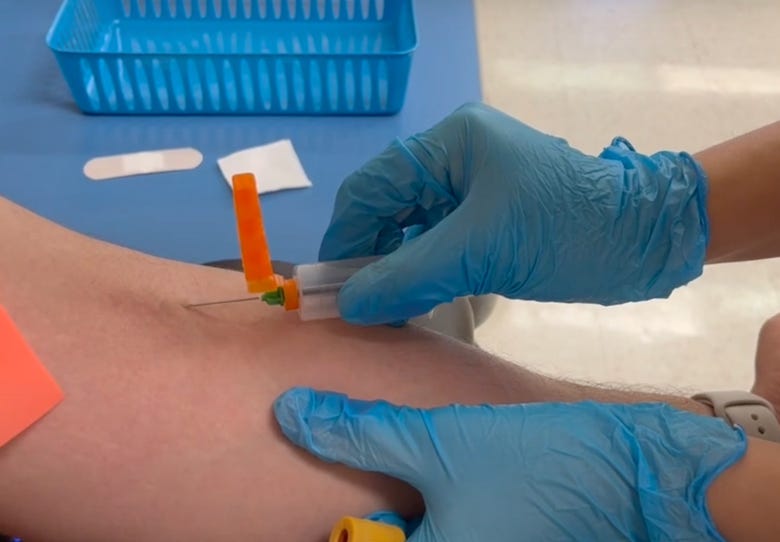
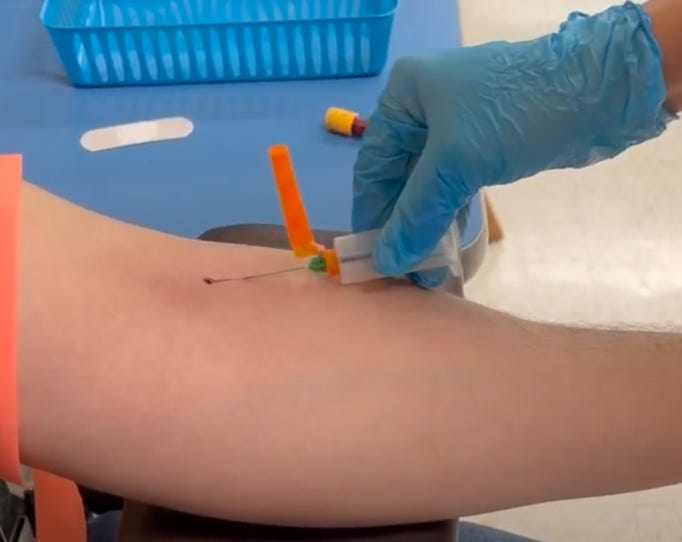
The Postanalytical phase:
Starts when the needle leaves the skin
Ends when the blood has been processed


A phlebotomist must never continue to the next phase if an error occurred in the current phase
,
