Chapter 5:
Special Collections, non-blood samples and Point-of Care Testing
PEDIATRIC PATIENTS:
Collecting blood from pediatric patients presents technical challenges. Because greater technical expertise is required to perform phlebotomy on children than on adults, you should master your collection methods on adult patients first. Similarly, you should master collection in older children before moving on to young children and infants.
SUPPLIES:
When performing venipuncture on children, use butterfly needles and smaller tubes to prevent iatrogenic anemia.
Take along a selection of rewards, such as stickers or small toys. Keep a stock of cartoon bandages as well.
Remember not to use these on infants younger than 2 years due to the danger of adhesive allergies.
ANESTHETICS:
Topical anesthetic cream may be useful for venipuncture procedures in pediatric patients. The most commonly used agent is EMLA (eutectic mixture of local anesthetics).
It must be applied 60 minutes before the draw, however, which means that the site must be chosen at that time. It is possible to numb more than one area if it is not practical to choose the site ahead of time.
GERIATRIC PATIENTS
With the aging of the population, many of your patients are likely to be geriatric patients. As with infants, collection from geriatric patients presents both physical and psychologic challenges.
PHYSICAL CHANGES:
As people age, their bodies undergo a number of changes that may have an impact on the safety and effectiveness of normal collection procedures.
Skin changes are among the most important. The skin becomes less elastic, and the layers of skin become thinner. Bruising is more likely, and it takes longer to replace cells, so longer healing times are needed.
Applying the Tourniquet:
If you are performing venipuncture, you can apply the tourniquet over clothing, a washcloth or paper towels to limit bruising.
Do not apply the tourniquet as tightly as you would normally, because veins in geriatric patients collapse more easily, and release the tourniquet immediately after inserting the needle.
To secure arm and comfort, you can place the arm on a phlebotomy wedge
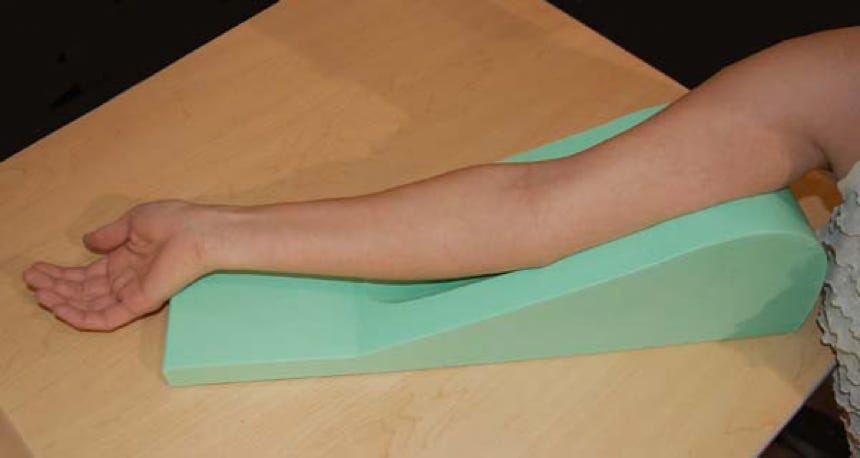
SPECIAL EQUIPMENT USED IN THE INTENSIVE CARE UNIT AND EMERGENCY ROOM
Patients in the ICU are likely to have some type of vascular access device or line in place that may affect your collection.
A vascular access device (VAD) is a tube that is inserted into either a vein or an artery and is used to administer fluids, medications or draw blood.
Blood collection from a VAD is done only by trained personnel on the physician's order, not by a phlebotomist.
TYPES OF VASCULAR ACCESS DEVICES:
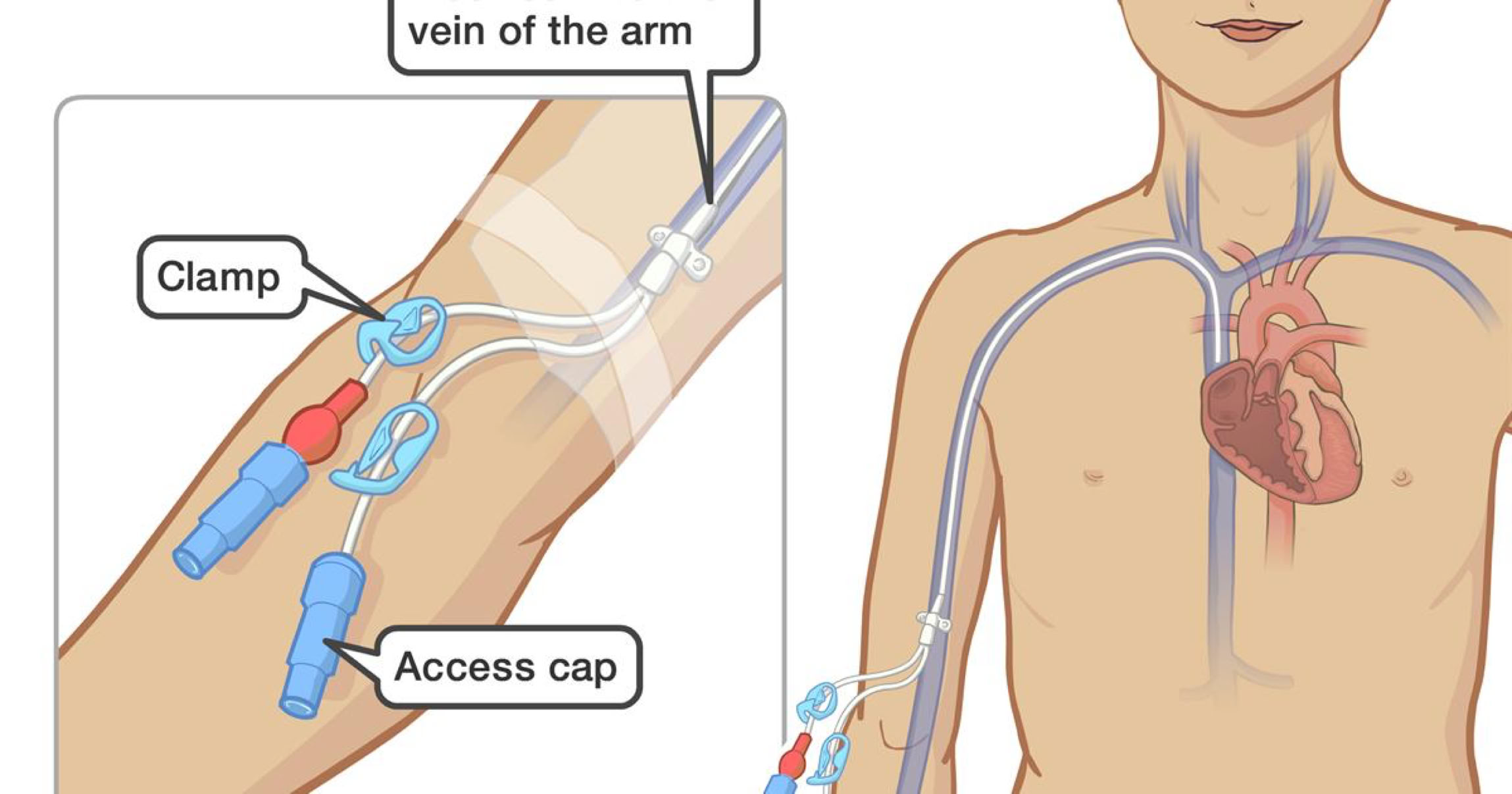
A central venous catheter (CVC), also called a central venous line is the most common type of VAD.
A peripherally inserted central catheter (PICC) is inserted into a central vein, usually from the antecubital area.
As stated earlier, only specially trained personnel can draw blood from a PICC Line, and a phlebotomist must never draw blood from these devices.
Arterial Punctures
Arterial Punctures are used in diagnosis & management of respiratory disorders
Personnel Who Perform Arterial Puncture
• Nurse
• Medical Technologist & technicians
• Respiratory Therapist
• Emergency medical technicians
Non-blood Specimens
Non-blood Specimens should be labeled with same ID information as blood specimens
Labeling should include type & source of specimen
Label should be applied to container, not lid, as lid is removed for testing
All body substances are potentially infectious
Standard precautions must be observed in handling them
Urine
Most frequently analyzed non-blood body fluid
Readily available, easy to collect & inexpensive to test.
Its analysis can aid in:
Monitoring wellness, Diagnosis & treatment of urinary tract infections and determining effectiveness or complications of therapy
Accurate results depend on:
Collection method
Container used
Specimen transportation & handling
Routine Urinalysis (UA)
It is the most commonly requested urine test. It screens for urinary & systemic disorders
Culture & Sensitivity
Ordered for patients with symptoms of urinary tract infection. Requires clean-catch collection in sterile container
1) Place measure portion of urine on special nutrient medium that encourages growth of microorganisms
2) Incubate for 18 to 24 hrs
3) Identify any microorganisms that grow
4) If microorganism is identified, sensitivity test is performed to determine which antibiotics will be effective
Urine drug screening performed to detect:
Illicit use of recreational drugs
Use of anabolic steroids to enhance performance in sports
Unwarranted use of prescription drugs
Tests are performed in groups based on drug classifications
Urine pregnancy testing
Tests for HCG, a hormone appearing in urine after conception
First morning specimen is preferred due to higher concentration
Types of Urine Specimens
Random: collected at any time
First morning/8-hour: collected on waking after 8hrs sleep
Glucose Tolerance test (GTT)
Urine Collection Methods
1) Regular Voided: patient voids into clean container
2) Mainstream: Patient voids into toilet first, then container
3) Midstream clean catch: requires cleaning of genital area before collection
4) Catheterized: sterile catheter inserted through urethra into bladder
5) Suprapubic aspiration: Collected by inserting needle directly into bladder 6) Pediatric: collected in plastic bag, for children not potty trained
Nasopharyngeal Secretions
From nasal cavity and pharynx
Cultured to detect presence of micro-organsims causing:
Diphtheria
Pertussis (whooping cough)
Covid-19
Collected using sterile Dacron or cotton tipped flexible wire swab. Swab is inserted into nose & passed into nasopharynx. It is rotated, removed, placed in sterile container, labeled, sent to lab
Sputum
Mucous or phlegm ejected from trachea, bronchi and lungs and is collected for diagnosis or monitoring of lower respiratory tract infectious (tuberculosis).
First morning specimens are preferred (larger volume).
Patient takes 3 or 4 deep breaths and then coughs forcefully, expelling sputum into container
Buccal (cheek) Swabs
Less invasive, painless alternative to blood collection for obtaining cells for DNA analysis
Phlebotomist gently massages mouth on inside of cheek with swab and DNA is extracted from cells on swab
Feces(stool)
Useful in evaluation of gastrointestinal disorders.
Stool specimens can be evaluated for presence of intestinal parasites & their eggs, Checked for presence of pathogenic bacteria & viruses and tested for presence of occult blood using guaiac test
Throat swabs
Collected to aid in diagnosis of strep infections. Nurses collect form inpatients, phlebotomists from outpatients
Collected with a sterile polyester-tipped swab in covered transport tube containing transport medium
.
