Infections are a significant cause of illness, Patients with weekend Immune Systems are particularly at risk for infection due to the increased severity of illness.
Infection control is one of the most important aspects of providing a safe environment for Patients. EKG Technicians must understand and follow the facility’s infection control policies and procedures.
The goal of infection control is to develop and maintain an environment that minimizes the risk of acquiring or transmitting infectious agents to hospital personnel, patients, and visitors.
It is not always possible for you to know if a patient is infectious or is incubating an infection. Therefore, it is important that you understand how infections occur and follow infection control practices and policies to protect yourself and your patients from infectious agents.
Infection:
When a microorganism invades the body, Multiplies, & Causes injury or disease.
Infection control:
Infection control measures practice in healthcare facilities to prevent and control the spread of disease
Pathogens:
harmful microorganisms capable of causing infection or disease
Pathogens include:
Bacteria
Fungi
Protozoa
Viruses
Chain of Infection:
For an infection to develop, each link of a chain must be connected. Breaking any link of the chain can stop the transmission of infection
CHAIN OF INFECTION
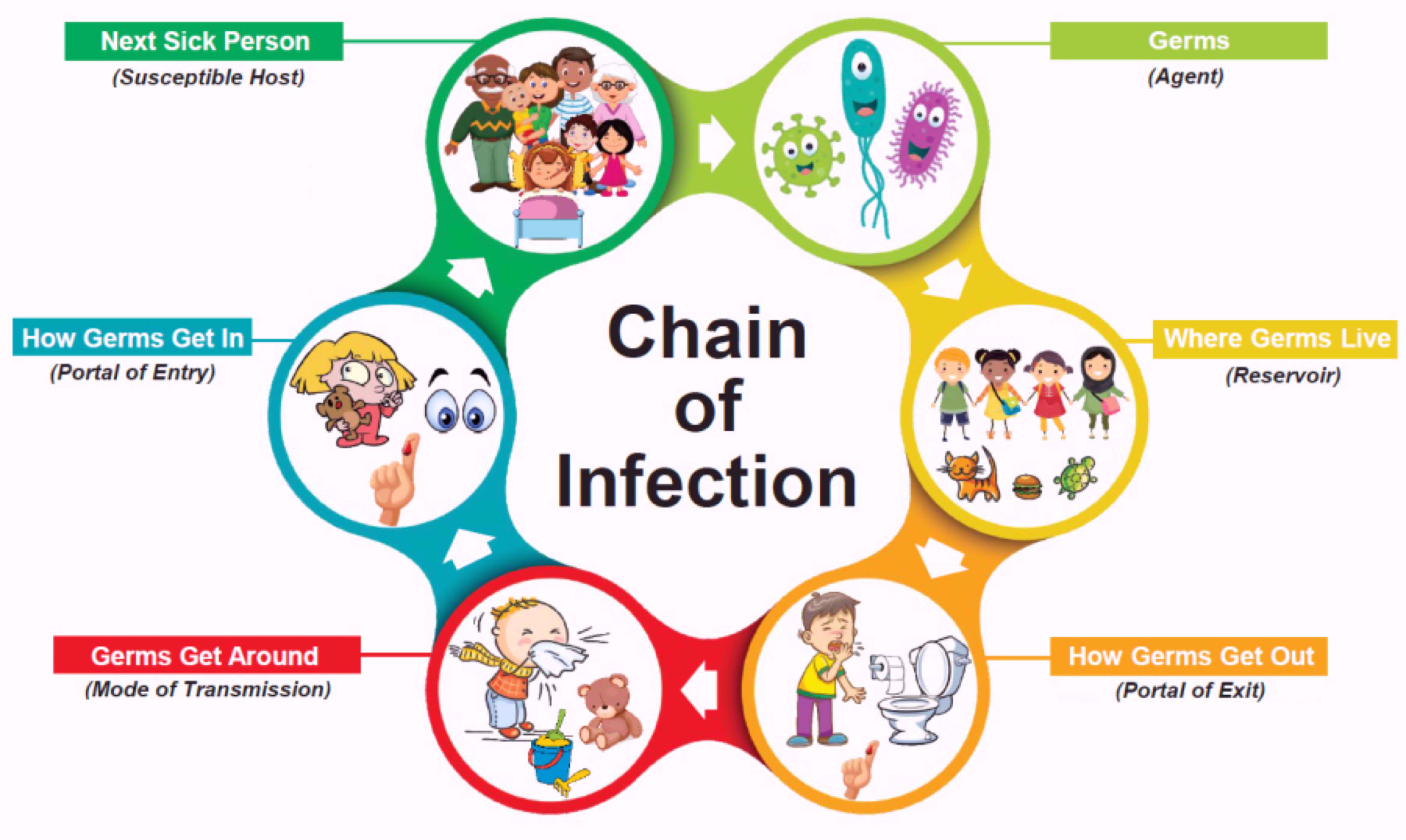
1. Infectious (causative) agent
- Pathogenic microbe responsible for causing an infection
2. Reservoir
- Source of infectious agent
-Place where microbe can survive & grow or multiply
- Includes: humans, animals, food, water, soil, equipment
3. Portal of exit
-A way an Infectious agent Is able to leave a reservoir host
-Secretions & exudates, tissue specimens, blood, feces, urine
4. Mode of transmission
- Airborne
- Contact
-Direct (touching, kissing)
- Indirect (contaminated objects)
- Droplet (coughing, sneezing)
- Vector (insect, arthropod, animal)
- Vehicle (food, water, drugs)
- Fomite (contaminated medical equipment)
5. Portal of Entry
- Way an infectious agent enters a susceptible host
-Includes: body orifices, mucous membranes, & breaks in skin
Mucous Membrane
The membranes that line body cavities, such as the mouth, nose, eyes, rectum and genitals
6. Susceptible host
- Someone with a decreased ability to resist Infection
- Factors: age, health, immune status
INFECTIONS
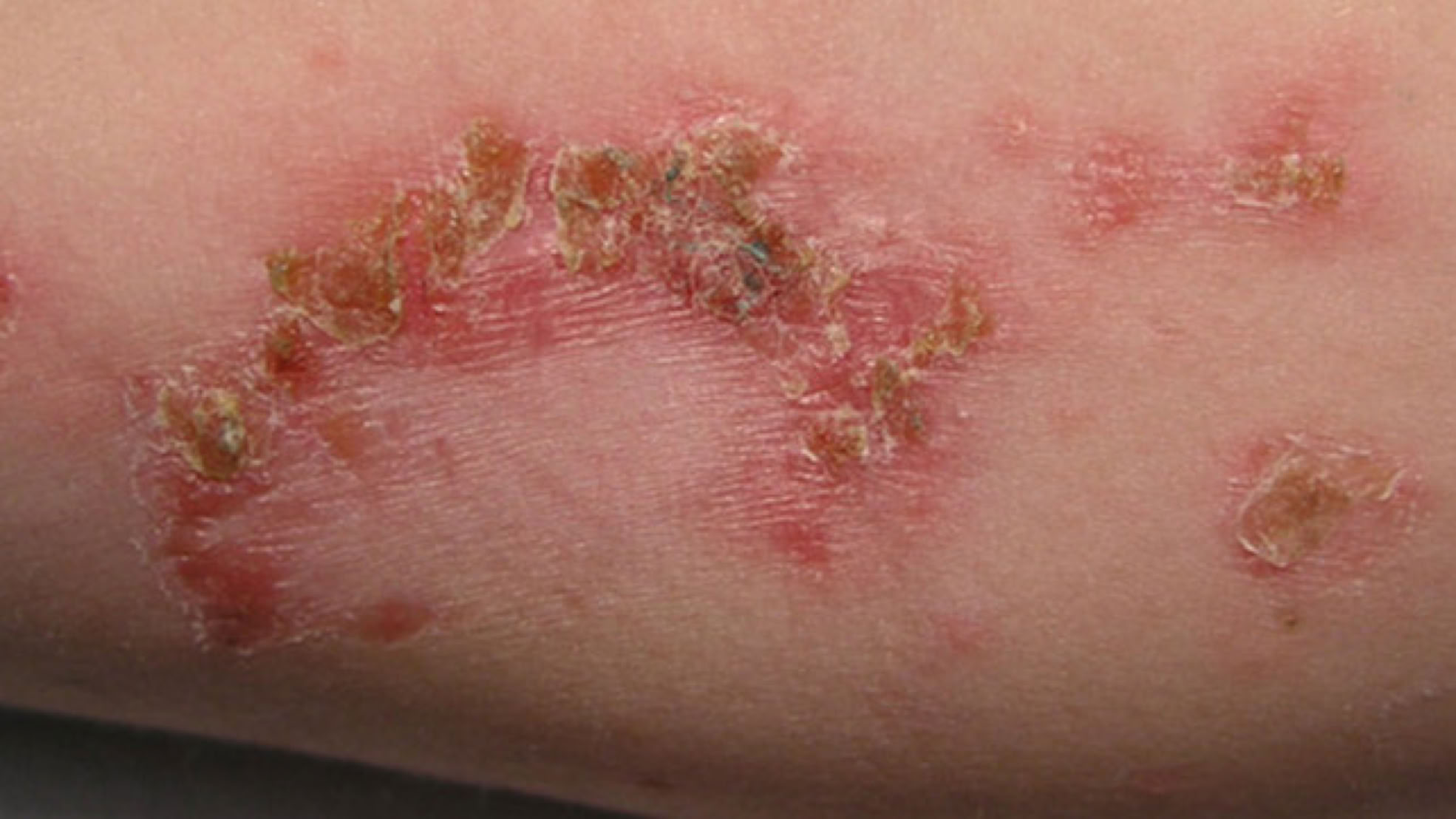
Types of Infections:
Localized infection:
an infection that is confined to a specific part of the body
Systemic infection:
an infection that is in the bloodstream and is spread throughout the body
Communicable:
Infections that are able to spread from person to person
Nosocomial or healthcare-associated Infections (HAIs)
infections that a patient has acquired within healthcare settings that result from treatment of other conditions, caused by infected personnel, patients, visitors, food, drugs, or equipment
GENERAL APPROACHES TO PREVENT AND CONTROL INFECTIONS

Medical asepsis (Clean Technique)
Practice(s) used to remove or destroy pathogens to prevent spread of infection from one person/place or object to another person/place or object.
Disinfection: The process of destroying pathogens on a surface. Even though it does not destroy all microbial spores, it greatly reduces the spread of infection by limiting microbial activity.
Sanitizing: means lowering the number of germs to a safe level.
Sterilization: free of all microorganisms (Pathogenic or not)
Washing hands with soap and water. This is the single most important practice to prevent the transmission of infection.
Some situations that require hand washing:
Anytime hands are visibly soiled
After personal use of the toilet
After contact with a Patient’s skin, mucous membranes or body fluid
After contact with any infectious materials
After removing gloves
After handling any soiled materials
Personal Protective Equipment

Personal protective equipment
• Gloves
• Gowns
• Lab coats
• Masks, face shields, & goggles
• Respirators
Universal precautions
Always treat blood & body fluids of all people as they are potentially Infectious
Used for all patients and is the #1 strategy for control of nosocomial infections.
Covers blood, all body fluids, skin breaks, and mucous membranes
Isolation Procedures:
- Keep patients with communicable infections separate from others
- Prevent spread of Infection
- Protect patients with compromised immune system
- Isolation requires doctor's order
- Infected patient are confined to private room
- Transmission-based precautions
• Used for patients known/suspected to have certain infections
• Three types: 1. airborne, 2. droplet, 3. contact
A EKG Technician will need to put on (don), gloves when caring for all patients, not only for a patient with a known communicable disease.
Gloves should also be donned when applying and removing electrodes on patients with open skin wounds or rashes. Gloves must be taken off and discarded immediately after providing care to avoid contamination. The EKG Technician should then wash his/her hands.
The use of these precautions is based on the illness the patient has and how it is spread to others. The precautions may be used separately or in combination, but they are always used in addition to standard precautions.
BLOOD BORNE PATHOGENS
OSHA (occupational safety health administration): the function of osha is to set standards to protect workers, provide safety education, inspect worksites, investigate workplace accidents, and set fines for safety violations.
The EKG Technician should be familiar with osha’s blood borne pathogens standard, which requires employers to protect healthcare workers from exposure to blood borne hazards.
Blood borne pathogens are microorganisms found in the blood that can cause infection and diseases (hepatitis B,C,HIV).
Blood that cannot be seen may be present in the body fluids or secretions even though the patient appears healthy.
Blood borne pathogen is a microorganism causing diseases by blood transmition.
General infection prevention guidelines that apply to all patients include the following:
OSHA Standards for Blood-Borne Pathogens (BBPs)
- Enforced by federal law
-Intended to reduce/eliminate occupational exposure to BBPs
Requires:
• Availability & use of PPE
• Special training
• Availability of vaccination for all at-risk personnel
Blood-Borne Pathogen
- Hepatitis B virus (HBV)
• Best defense: HBV vaccination
• HBV exposure hazards
• Present in blood & other body fluids
• can survive up to a week on objects
• Transmitted via needle sticks, sexual contact
-Hepatitis C virus (HCV)
• HCV exposure hazards
• Present in blood & serum; sometimes saliva
• Infection primarily occurs after large or multiple exposures
• Transmitted via needle sticks, sexual contact
• BBP Exposure Routes
- Skin is pierced by a contaminated needle or sharp object
- Blood or other body fluid splashes In eyes, nose, or mouth
- Blood or other body fluid contacts cut, scratch, or abrasion
- A human bite breaks the skin
Biohazards:

Osha requires disposal of infectious and hazardous waste according to safety standards.
Biohazard containers: are used for the disposal of waste that may be contaminated with pathogens that presents a danger to people, including sharp objects. The biohazard containers are considered full when they are ¾ full.
AREA DECONTAMINATION

Cleanup of Body Fluid Spills
- EPA-approved chemical solutions & kits
- Gloves must be worn
- Absorb material without spreading it over wider area
Biohazard Waste Disposal
- All non-reusable items contaminated with blood or body fluids go in biohazard waste containers
Surface Decontamination (required by OSHA)
- All surfaces In specimen collection & processing areas
- 1:10 bleach solution or other disinfectant approved by EPA
Material Safety Data Sheet

Safety data sheet: include information such as the properties of each chemical. protective measures; and safety precautions for handling, storing, and transporting the chemical.
Every Chemical used in your facility will have a MSDS in the MSDS Binder.
Every EKG Tech must know the location of the MSDS Binder in their facility in case of an emergency situation.

